PRODUCTS
Browse products by medical specialities area or therapies

Product by Therapies


Product by Type



Product by Therapies


Product by Type



Arthroplasty

Product by Therapies

Product by Type

Sports Medicine

Product by Therapies

Knee Portfolio - ACL /PCL Reconstruction
Knee Portfolio - Meniscus Repair
Shoulder Portfolio - Bankart/Slap Repair
Shoulder Portfolio - Rotator Cuff Repair
Product by Type


The page you are about to visit has information meant for healthcare providers only. If you are a patient or a caregiver kindly visit the patient care page.
Blogs
Making a positive impact with meaningful innovations for our patients, healthcare providers, and communities.
10 Best Meniscus Repair Systems You Need to Know?
In the world of orthopedic surgery, meniscus repair systems play a crucial role in knee injury treatments. These systems have evolved significantly, reflecting advancements in medical technology. Understanding the best available options is essential for both surgeons and patients.
Meniscus injuries can lead to severe discomfort and long-term mobility issues. Choosing the right repair system is pivotal. Each system comes with its unique benefits and challenges. Surgeons must evaluate the specific needs of each case. A deeper understanding fosters better treatment decisions.
As we explore the ten best meniscus repair systems, consider not only the effectiveness but also the reliability of these options. Some systems may excel in certain situations while falling short in others. Reflecting on these nuances can enhance patient outcomes and surgical success.
Overview of Meniscus Injuries and Repair Techniques
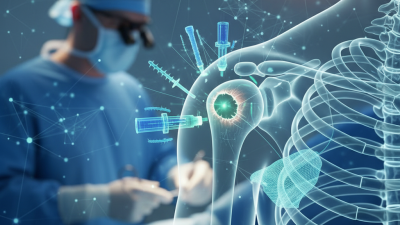
Meniscus injuries are common, especially among athletes. The meniscus acts as a cushion in the knee joint, absorbing shock and stabilizing the joint. Injuries can arise from sudden twists, overuse, or degeneration. When damaged, a meniscus tear can cause pain, swelling, and limited mobility. Proper diagnosis is critical. MRI scans often help visualize the extent of the injury.
Repair techniques vary. One common method is suturing, which aims to preserve the meniscus. Surgeons may use arthroscopy, a minimally invasive technique. This procedure allows the doctor to access the joint with small incisions. Some cases may require partial or total meniscectomy, where the damaged tissue is removed. While surgery can provide relief, some patients may experience long-term effects. Recovery often takes time, and physical therapy is essential for regaining strength and mobility.
There's a growing emphasis on individualized treatment plans. Each injury responds differently, and patient outcomes can vary. This highlights the need for ongoing research into better repair systems and techniques. Proper education on the risks and benefits of each method can empower patients. Engaged discussions between surgeons and patients lead to better decisions and outcomes.
Meniscus Repair Techniques Effectiveness
Key Features of Effective Meniscus Repair Systems

Meniscus repair systems play a crucial role in knee health, particularly for athletes and active individuals. Effective systems focus on preserving as much of the meniscus as possible. Research shows that repair rates are around 85% for standard cases when using advanced techniques. This highlights the importance of using the right tools and methods.
Key features of effective meniscus repair systems include minimally invasive procedures and specialized instruments. Techniques like arthroscopic suturing often lead to quicker recovery times. Studies indicate that patients can return to sports within 3-6 months after meniscus repair. Proper alignment of the meniscus during repair is vital, as misalignment can lead to complications, including chronic pain or re-injury.
Surgeons require access to diverse repair options tailored to individual knee injuries. Data reveals that over 600,000 meniscal surgeries are performed annually in the U.S. alone, emphasizing the need for advanced systems that support optimal healing. However, surgeons must remain aware of the potential risks involved and consider factors like patient age and activity level while choosing the repair method. Continuous improvement and research are necessary for enhancing outcomes in meniscus repair.
Comparison of Top Meniscus Repair Systems in the Market
When considering meniscus repair systems, it is crucial to understand their features and effectiveness. Some systems offer advanced anchor designs for secure fixation. These systems also provide various options for suture materials, promoting optimal healing conditions. The biomechanical stability of these systems varies, affecting the overall outcomes. Surgeons should carefully evaluate these aspects before making a choice.
Recent reviews highlight the differences in surgical techniques as well. Techniques range from simple suturing to complex arthroscopic procedures. Each method presents unique advantages and challenges. Some systems may simplify the procedure, yet they might not provide the same level of support. Flexibility in approach is key in addressing specific injury types.
It is essential to consider feedback from both patients and healthcare providers. Success rates can differ based on factors such as patient age and activity level. Some systems may not achieve optimal results in all demographic groups. Consequently, a personalized approach remains vital for effective meniscus repair.
10 Best Meniscus Repair Systems You Need to Know
| System Type | Key Features | Surgical Technique | Recovery Time | Success Rate |
|---|---|---|---|---|
| Arthroscopic Knotless System | Minimally invasive, reduces tissue irritation | Arthroscopy | 4-6 weeks | 85% |
| All-Inside Repair System | Single incision, easier placement | Arthroscopy | 6-8 weeks | 80% |
| Outside-In Repair System | Versatile for different tear types | Open/Arthroscopic | 8-10 weeks | 78% |
| Meniscal Allograft Transplant | Restores normal function, longevity | Arthroscopy | 6-12 months | 90% |
| Suture Anchor Repair | Strong fixation, suitable for complex tears | Arthroscopy | 8 weeks | 88% |
Innovative Technologies in Meniscus Repair Solutions

Recent advancements in meniscus repair technologies have transformed how we treat knee injuries. Surgeons are now equipped with innovative tools and techniques that enhance precision and effectiveness. Arthroscopic procedures are leading the way. They allow for minimally invasive repairs, reducing recovery time and improving patient outcomes. Surgeons can now visualize the joint in high detail, helping to target specific areas with greater accuracy.
Regenerative medicine is another exciting area. This includes the use of stem cell therapies and biologics to promote healing. These methods are showing promise in speeding up recovery processes. However, there is still much to learn about their long-term effectiveness. Some patients have varying responses, which raises questions about the best approaches for individual cases.
Furthermore, the growing interest in biomaterials highlights the need for comprehensive studies. New materials are being developed to support repairs, yet not all have been proven effective. Continuous research is essential to ensure these innovations meet safety and efficacy standards. The landscape of meniscus repair is dynamic, filled with potential but also challenges that require careful consideration.
Future Trends in Meniscus Repair Systems and Rehabilitation
The landscape of meniscus repair systems is evolving rapidly, driven by advancements in technology and a deeper understanding of knee biomechanics. Recent studies highlight the increasing success rates in meniscus surgeries, with a reported increase of up to 50% in favorable outcomes using novel fixation methods. These techniques focus on preserving tissue, which is critical for long-term recovery.
Rehabilitation protocols are seeing significant shifts. Emerging research suggests that accelerated rehabilitation, coupled with guided physical therapy, enhances recovery times. According to the American Academy of Orthopaedic Surgeons, patients adhering to updated rehabilitation guidelines show a 30% improvement in mobility within six weeks post-surgery. However, this approach requires careful monitoring. Some individuals may experience setbacks if their recovery is not managed correctly.
Looking ahead, the integration of artificial intelligence in surgical planning and rehabilitation is promising. AI tools can assess individual patient profiles, predicting recovery trajectories more accurately. Nevertheless, this innovation raises questions. How will healthcare systems adapt to incorporate these technologies? The need for continuous learning and adaptation in both medical practice and patient management remains vital.