PRODUCTS
Browse products by medical specialities area or therapies

Product by Therapies


Product by Type



Product by Therapies


Product by Type



Arthroplasty

Product by Therapies

Product by Type

Sports Medicine

Product by Therapies

Knee Portfolio - ACL /PCL Reconstruction
Knee Portfolio - Meniscus Repair
Shoulder Portfolio - Bankart/Slap Repair
Shoulder Portfolio - Rotator Cuff Repair
Product by Type


The page you are about to visit has information meant for healthcare providers only. If you are a patient or a caregiver kindly visit the patient care page.
Blogs
Making a positive impact with meaningful innovations for our patients, healthcare providers, and communities.
How to Ensure Tibial Implant Rotational Stability in Knee Surgery?
Tibial implant rotational stability is crucial in knee surgeries. The proper alignment and fixation of the tibial component can determine the longevity of a knee implant. Surgeons often face challenges in achieving optimal rotation, impacting the patient's overall functionality post-surgery.
Various factors influence tibial implant rotational stability. These include surgical techniques, implant design, and patient anatomy. Experience plays a vital role in addressing these complexities. Surgeons must be aware of the nuances that impact stability. They need to consider specific patient factors, such as bone density and knee mechanics. Insufficient attention to these details may lead to complications.
Understanding the biomechanical principles behind tibial implant rotational stability is essential. Innovations in implant design provide options for improved stability. However, no single solution fits all cases. Surgeons must remain adaptable and critical in their approach. Continuous evaluation and learning from each procedure can enhance skills and outcomes.

Factors Influencing Rotational Stability of Tibial Implants in Knee Surgery
Ensuring the rotational stability of tibial implants during knee surgery is crucial for patient outcomes. Several factors influence this stability. Proper alignment and positioning of the implant play a significant role. An accurate anatomical fit minimizes rotational forces during movement.
The quality of bone stock can also affect stability. Deteriorated or insufficient bone can lead to compromised implant fixation. Surgeons must assess bone integrity before deciding on the type of implant and fixation technique. Techniques such as using supplemental fixation devices may enhance stability, yet they require careful planning.
Surgeon technique and experience matter too. Ensuring proper surgical techniques, including soft tissue balance, can impact the longevity of the implant. A well-balanced knee reduces stress on the implant. Regularly revisiting and analyzing surgical outcomes fosters continuous improvement. Each case offers insights that can refine future procedures.
Importance of Surgical Technique in Achieving Rotational Stability
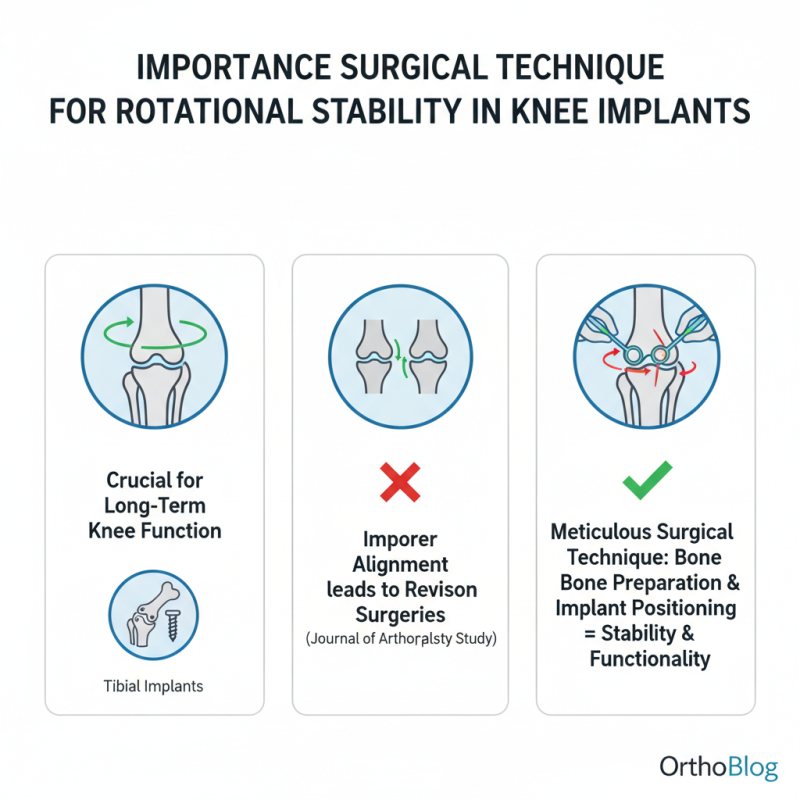
Achieving rotational stability in tibial implants is crucial for long-term knee function. A study published in the Journal of Arthroplasty highlighted that improper alignment can lead to an increase in revision surgeries. Surgical technique significantly affects the success of achieving proper alignment. Surgeons must be meticulous in their bone preparation and implant positioning to secure stability and functionality.
One common challenge is the variability in patient anatomy. Different bone structures may require unique approaches. Ensuring accurate cuts and consistent measurements can help address this issue. A recent report noted that 25% of knee replacements face complications due to malalignment. Thus, utilizing advanced imaging techniques during surgery may enhance precision.
Here are some tips for achieving optimal rotational stability:
- Always verify alignment with intraoperative imaging.
- Employ trial components to assess fit before finalizing the implant.
- Encourage ongoing education and training for surgical teams to stay updated on best practices.
These strategies can guide surgeons toward better outcomes while confronting the complexities of knee surgery.
Material Properties and Their Role in Tibial Implant Stability
The stability of tibial implants in knee surgery hinges significantly on material properties. A recent study highlighted that the mechanical strength and wear resistance of materials used can directly influence implant longevity. For instance, titanium alloys exhibit remarkable fatigue resistance, with reported endurance limits up to 900 MPa in some applications. This strength is essential in minimizing micro-movement during the healing process, thus reducing the risk of failure.
In addition to strength, the surface roughness of tibial implants plays a critical role in stability. Profiles that provide optimal friction can enhance initial fixation. Research indicates that surfaces with a roughness average of 1-2 micrometers show an increased ability for osseointegration. However, achieving the right balance between roughness and smoothness is challenging. Excessively rough surfaces can lead to stress risers, making the implant more susceptible to cracking.
Material fatigue is another element to consider. Implants endure continuous cyclic loading, which can lead to gradual material degradation. Studies have noted that specific polymers used in spacers may lose approximately 10-30% of their initial mechanical properties over time. Addressing these factors is essential for improving implant design and ensuring a more stable outcome for patients. Continuous research needs to address these material limitations for future advancements.
How to Ensure Tibial Implant Rotational Stability in Knee Surgery? - Material Properties and Their Role in Tibial Implant Stability
| Material Type | Elastic Modulus (GPa) | Yield Strength (MPa) | Ultimate Tensile Strength (MPa) | Fatigue Limit (MPa) | Coefficient of Friction |
|---|---|---|---|---|---|
| Titanium Alloy | 110 | 800 | 950 | 400 | 0.25 |
| Cobalt-Chromium Alloy | 210 | 620 | 800 | 350 | 0.35 |
| High-Density Polyethylene (HDPE) | 1 | 20 | 30 | 12 | 0.2 |
Impact of Alignment and Positioning on Tibial Component Rotation

Ensuring tibial implant rotational stability is a significant challenge in knee surgery. The tibial component's alignment and position directly influence its rotational stability. When the alignment is off, it can lead to instability and discomfort for the patient. Surgical precision is crucial for optimal outcomes.
Tips for alignment include using intraoperative imaging. It assists in verifying the correct tibial component placement. Properly checking the alignment can decrease complications. A thorough assessment of the limb’s alignment pre-surgery can also provide valuable insights. Aim for a symmetrical balance during the procedure.
Positioning during the operation plays a role in stability as well. Achieving a neutral position may help reduce the risk of malrotation. A detailed discussion with the surgical team about the approach is essential. Reflection on previous cases can help recognize common pitfalls. Learning from mistakes ensures continuous improvement for future surgeries.
Post-Operative Rehabilitation Strategies to Maintain Implant Stability
Post-operative rehabilitation is crucial for maintaining tibial implant stability in knee surgery. Engaging in structured physical therapy is essential. Customized exercise plans can significantly enhance recovery. These routines should focus on strength, flexibility, and range of motion. Simple exercises like quadriceps strengthening can be highly effective. They help stabilize the knee joint and prevent implant loosening.
Weight-bearing activities are another vital aspect. Slowly increasing activity levels promotes bone healing. Patients should carefully monitor their pain levels during these exercises. This can guide them in adjusting their rehabilitation regime. Engaging in low-impact activities, such as swimming or cycling, can also be beneficial. Yet, a focus on proper form is necessary to avoid injury.
Education is key in post-operative recovery. Patients must understand the importance of adhering to their rehabilitation plan. They should also recognize early signs of instability, such as unusual pain or swelling. Regular follow-ups with healthcare providers can pinpoint any issues quickly. This proactive approach helps maintain long-term implant stability. It's essential to reflect on their progress and adapt strategies as needed.
Related Posts
-
2026 Best Tibial Implant Rotational Stability Solutions and Innovations?
-
What is Bioabsorbable Interference Screws and Their Benefits?
-
China Top Freedom of Movement Implants Enhancing Mobility and Lifestyle?
-
Top 10 Shoulder Bankart Repair Systems You Should Know?
-
What is Total Knee Replacement Systems and How Do They Work?
-

2026 How to Achieve Knee and Hip Motion Restoration Effectively?